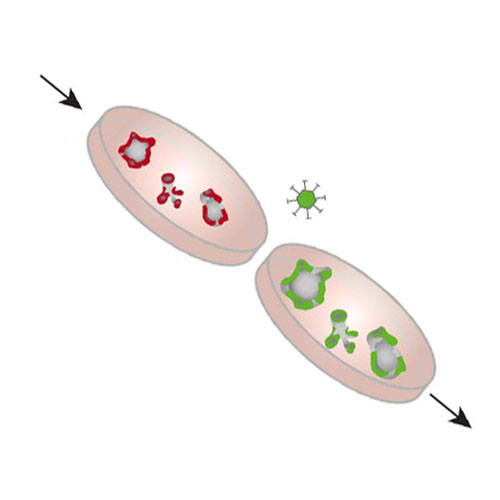
Stem Cell–Derived Photoreceptor Transplants Differentially Integrate Into Mouse Models of Cone-Rod Dystrophy
20-Jun-2016
Investigative Ophthalmology & Visual Science, Vol.57, Issue 7, 3509-3520. doi:10.1167/iovs.16-19087
IOVS, online article
Purpose: Preclinical studies on photoreceptor transplantation provided evidence for restoration of visual function with pluripotent stem cells considered as a potential source for sufficient amounts of donor material. Adequate preclinical models representing retinal disease conditions of potential future patients are needed for translation research. Here we compared transplant integration in mouse models with mild (prominin1-deficient; Prom1−/−) or severe (cone photoreceptor function loss 1/rhodopsin-deficient double-mutant; Cpfl1/Rho−/−) cone-rod degeneration.
Methods: For photoreceptor transplant production, we combined the mouse embryonic stem cell retinal organoid system with rhodopsin-driven GFP cell labeling by recombinant adeno-associated virus (AAV). Organoid-derived photoreceptors were enriched by CD73-based magnetic-activated cell sorting (MACS) and transplanted subretinally into wild-type, Prom1−/− and Cpfl1/Rho−/− hosts. The survival, maturation, and synapse formation of donor cells was analyzed by immunohistochemistry.
Results: Retinal organoids yielded high photoreceptor numbers that were further MACS-enriched to 85% purity. Grafted photoreceptors survived in the subretinal space of all mouse models. Some cells integrated into wild-type as well as Prom1−/− mouse retinas and acquired a mature morphology, expressing rod and synaptic markers in close proximity to second-order neurons. In contrast, in the novel Cpfl1/Rho−/− model with complete photoreceptor degeneration, transplants remained confined to the subretinal space, expressed rod-specific but only reduced synaptic markers, and did not acquire mature morphology.
Conclusions: Comparison of photoreceptor grafts in preclinical models with incomplete or complete photoreceptor loss, showed differential transplant success with effective and impaired integration, respectively. Thus, Cpfl1/Rho−/− mice represent a potential benchmark model resembling patients with severe retinal degeneration to optimize photoreceptor replacement therapies.